Why Simulation-Based Training Is Essential in Healthcare Education
Key Takeaways
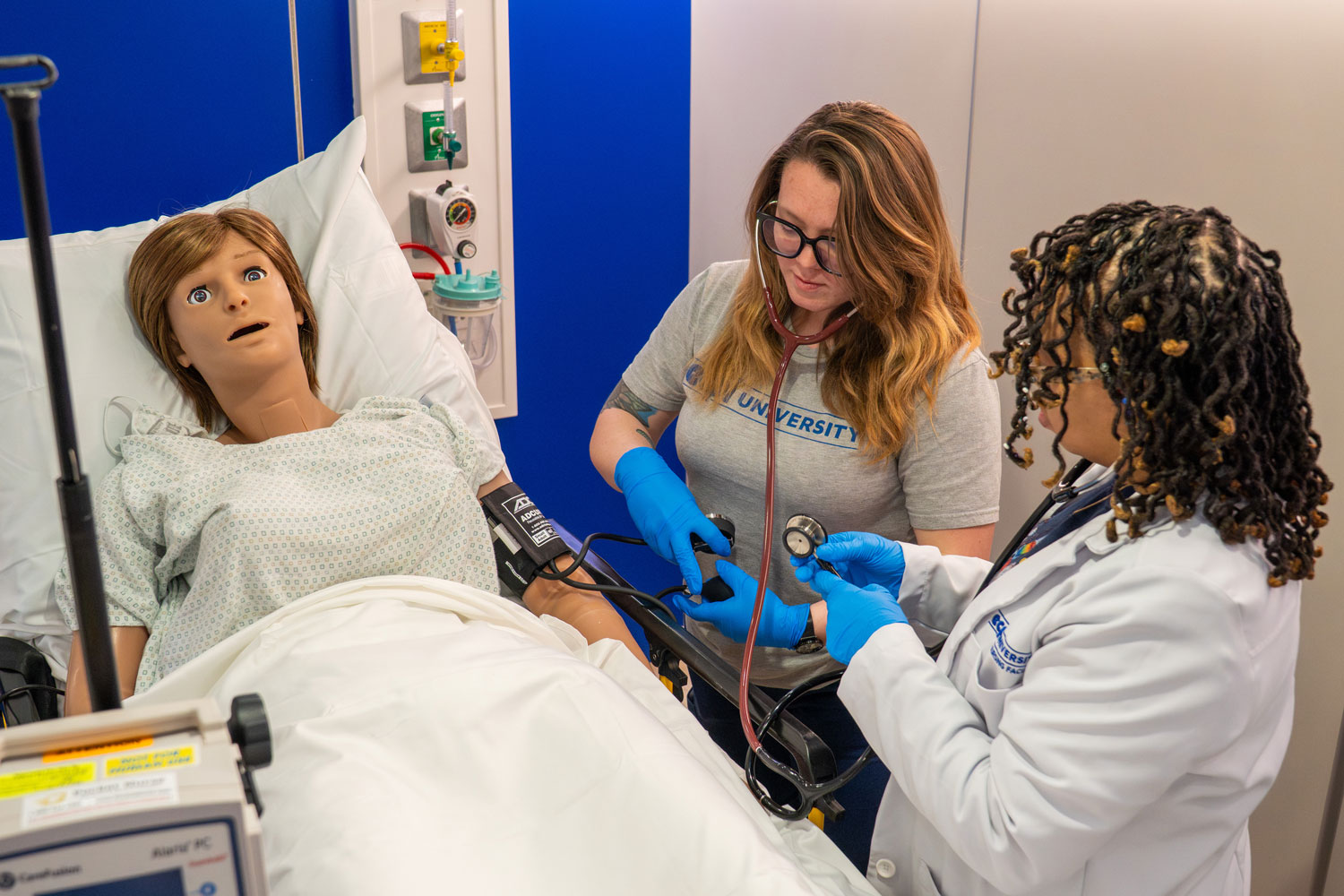
Simulation-based training reduces hesitation and builds readiness by giving healthcare students hands-on experience with equipment and clinical decision-making before patient care, bridging the gap between learning and real-world practice. Clinical simulations with hospital beds and patient monitoring systems prepare graduates to function immediately in clinical settings without initial trial-and-error.
- Simulation environments replicate hospital equipment and workflows including patient monitors, IV administration, wound care procedures, and medication administration systems, enabling muscle-memory development before patient contact
- Clinical decision-making practice in simulated scenarios builds recognition of patient status changes, emergency protocols, and triage processes, preventing hesitation when similar situations occur with actual patients
- Hospital bed familiarity and equipment handling during simulations reduce startup time in real clinical settings, allowing new graduates to focus on patient assessment and care rather than equipment operation
- Patient monitor systems and vital sign interpretation practice in simulations ensure students understand normal and abnormal waveforms, alarms, and clinical significance before monitoring real patients
- Simulation-based learning reduces distance between classroom instruction and bedside practice, allowing students to enter clinical rotations with foundational competency and functional readiness
In healthcare education, realism carries a vital and practical purpose. Students are preparing for roles in settings where equipment and judgment both matter at once. The closer training comes to these conditions, the less room there is for hesitation when graduates step into patient care.
That expectation feels obvious now, but it was something built over time. John Taylor, a 1996 ECPI University graduate, has watched that shift firsthand. His career has taken him from military service to biomedical training to hospital systems, and now back to the university as an industry partner helping shape clinical learning spaces.
How Training Moved from Catching Up to Keeping Pace
When Taylor arrived at ECPI in 1994 after leaving the Navy, the technology in the classroom reflected a different era. Students worked on bulky computer stations with CRT monitors and 3.5-inch floppy disks, and the biomedical equipment in the labs was still being built out.
But change was quickly underway. Over his two years at ECPI, Taylor saw how quickly the program was evolving in real time. He recalls students, faculty, and staff moving new lab equipment through doors while parts of the building were still being remodeled. "All the students jumped right in," he says. "I felt like we were part of the school growing."
While other colleges of the time leaned on classroom theory and lecture-based instruction, ECPI's goal was clear: keep training as close as possible to what students would encounter when they graduate.
That decision paid off. When Taylor walked into Sentara General Hospital, the equipment and software they were using felt familiar because they were part of his program. The experience ultimately secured him an internship.
That was 30 years ago. In today’s healthcare settings, that kind of alignment is less a competitive advantage and more a baseline. As the field grows more complex and technology is more integrated, the expectation is that students will arrive ready to function within the setting.

Why Realistic Simulation Matters
Clinical training works best when it reduces the distance between learning and doing. A student who has already handled a hospital bed or learned the logic of a patient monitor enters a clinical setting with a different level of readiness than someone encountering those systems for the first time. In many cases, that familiarity is what separates observation from participation.
The stakes are also not abstract. Readiness influences performance in real clinical environments. That in turn is directly tied to outcomes, because mistakes are no longer theoretical once a patient is involved, and sometimes there is no option to reset and try again.
Training on equipment that mirrors the field helps students build that familiarity before the pressure is real. It allows them the safety net of being able to make mistakes and correct them. This experience strengthens both their technical skills and their ability to respond under pressure.
As Taylor puts it, "You're not just doing a job. You're training people to save your life. That nurse that goes to school here is going to be at Sentara. She better know that infusion pump."
From Student to Industry Partner
Taylor's role today reflects a different kind of connection to the university. After building experience across hospital environments, he now runs his own company, iMedical Healthcare Solutions, which supplies and services clinical equipment for health systems across the region. It counts ECPI University among its longest-running clients.
His work is grounded in what hospitals are actually using, from ICU environments to surgical settings. That perspective helps ensure training spaces reflect current practice rather than outdated assumptions.
He started as a student learning on equipment that was still evolving, and now returns as a partner helping determine what that equipment should be. There is something rare and unique about that progression: a graduate whose training shaped him, coming back to shape the training.
When former students contribute to the environments where future students learn, the value of that original education extends well past graduation.

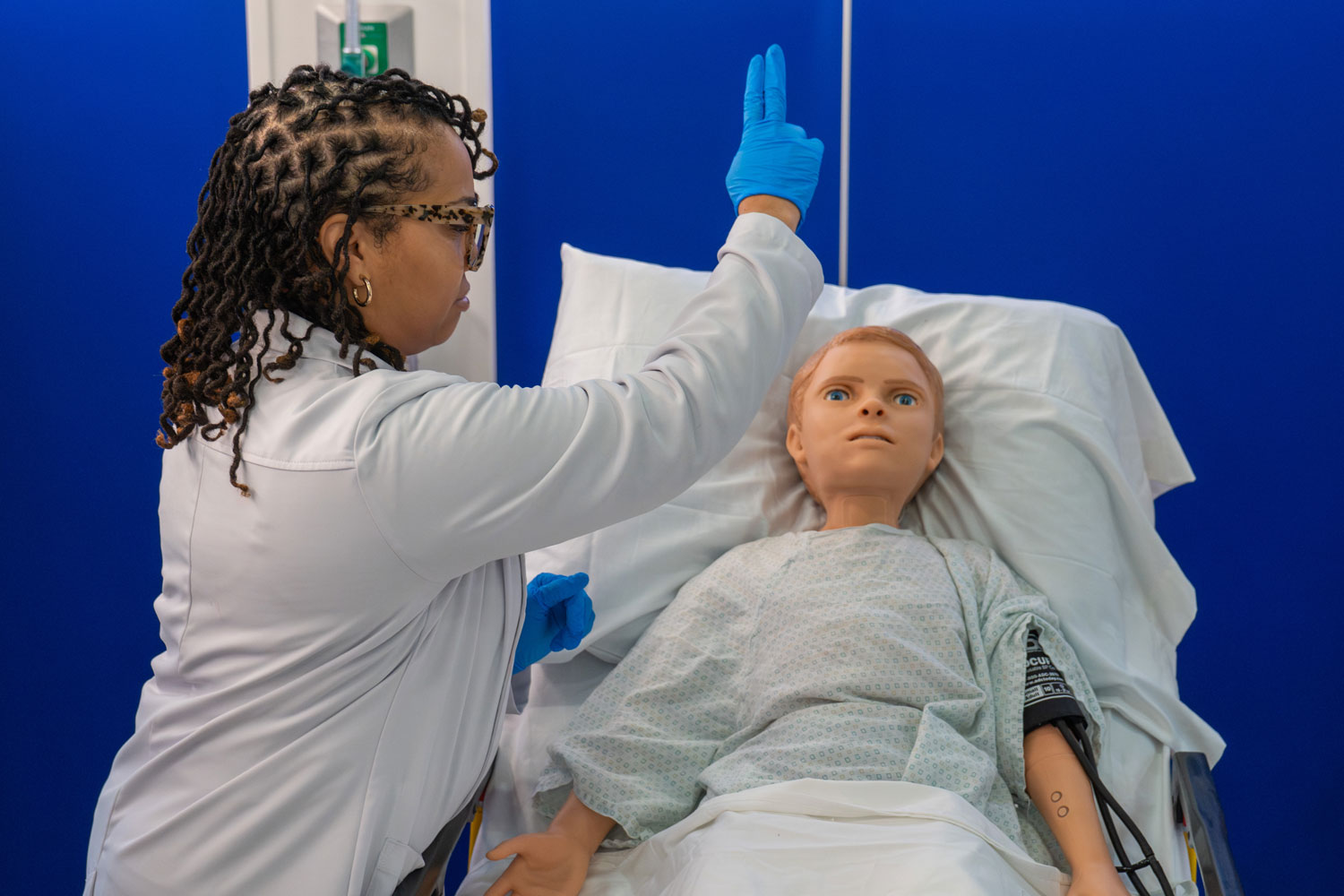
Simulation in Practice
Recent investments in simulation-based training spaces show how far this approach has developed. At ECPI's Manassas campus, ICU simulation and radiology labs were designed to reflect real clinical environments, giving students access to the same types of systems they will encounter in the field. Similar ICU training environments are now being developed at other campuses, including Orlando.
Taylor has been closely involved in these efforts, helping supply and install equipment while advising on what accurately reflects current hospital environments. His perspective comes from years spent in ICUs, operating rooms, and clinical facilities, where the details of layout and equipment directly shape how care is delivered.
That level of realism reflects a broader shift in expectations. Training environments are no longer treated as separate from practice, but as an extension of it.
The goal, as he frames it, is not to approximate a hospital setting but to recreate it. "These are the same beds at Sentara, the same infusion pump, the same manikins. Everything you're going to touch in the hospital. It's real here."
When new equipment arrives, Taylor says their reaction speaks volumes. "It’s like Christmas. They say, 'Oh my gosh, look at those beds.'" They ask how everything operates, why certain things are there, and what each piece does. That curiosity signals that the learning environment is working.

What This Means for Career-Focused Education
As healthcare continues to evolve, training environments have to keep pace. The expectation is already clear: students are not entering clinical settings to figure things out for the first time. They are expected to function within them from the start.
That level of readiness depends on how closely training reflects real practice. Simulation-based environments give students direct experience with the equipment and decision-making they will encounter before real patient care is involved.
For career-focused programs, that level of preparation is a clear indicator of how well they reflect the demands of the field. Thirty years from now, the technology and the equipment in healthcare will look very different. The approach and the willingness to adapt will need to remain the same.
